“Compassion is showing our scars to those with open wounds.” –Gary Hallquist
Dear Lindsey,
In my last letter, I gave Part I to this story. I originally hesitated from sharing this brain tumor journey: Was I afraid of dwelling in the past? Was I afraid I would scare readers into getting themselves checked for brain tumors? Or was it that my heart aches for so many people still in their “Holland,” with worse problems, bigger tumors, cancer in multiple family members, unrelenting back pain, life-changing car accidents, addictions, etc., but they are still living through them today? A friend reminded me that suffering is not a competition. If showing our scars can be helpful to those with open wounds, then sharing the past is celebrating God’s victories. So I continue to write:
When we last left the story, my insurance application had been rejected unless I would get another brain MRI.
September 6, 2008
I had the MRI early in the morning. I “checkmarked the box” so I could get the new insurance. The diagnostic center gave me the normal line about how I would hear from my doctor within two weeks to review the results. I knew from booking this appointment that the neurosurgeon was on vacation that week, so my follow-up appointment to review the MRI was scheduled for September 22. I was not worried, just like she had told me not to be at my previous appointment, months earlier.
The following week, the caller ID revealed the hospital’s number on a phone call. The kind woman told me that they needed to get another scan for clarity.
“I am flying to Salt Lake City in the morning,” I told her and we booked a time for the following Monday and ended our call. I figured my brain must have moved during its photo shoot, and blurred their view. (smile) It’s hard to hold still for 45 minutes – even if your head IS clamped.
The phone rang again within minutes. “I spoke with your doctor, and she said you should not get on the plane.”
“Is something wrong?” The dumb question escaped my mouth as my nerves escalated, realizing they had called that doctor on vacation –obviously, something was wrong.
“No, we just need a better view. It is actually not an MRI, but a VRI we will be taking,” she said as if that was a logical answer to my panicked question.
“So why can’t I fly? Is it the plane pressure? I am supposed to leave at 10am.”
“Well you could come in at 7am, and if the radiologist clears you, you could be out in plenty of time to make your plane.”
The following morning, I went back on the cold table into the tube. It screamed a sound similar to the old dot-matrix printer, seemingly through a microphone directly into my ears. Halfway through the test, the young (and obviously naïve) technician started my IV as normal and asked,
“So how long have you known about this?”
Known about what?! Went through my head, but I played it cool: “A while,” I said, not sure if we were talking about the same thing.
“Can they operate?” she asked, curious.
Oh. My. Word. Am I in a Twilight Zone? Did I miss a phone call somewhere? Last I had heard, this kind of tumor is common and no big deal… “Uh, I don’t know yet. I think that’s why I’m here,” my heart began to race as my mind wandered in “what ifs,” but exteriorly, I was calm.
“Is it cancer?” she asked me.
“I hope not,” I said quickly, as if the speed of my answer would bat that chance away.
“Well, you must be scared,” she said as she rolled the table with me on it back into the tube.
I lay on the hard, skinny table surrounded by my own cocoon for the second 20-30 minutes of the test. I thanked God that the technician was talking to me and not to some little old lady who didn’t know my God of peace. I knew the tech wasn’t supposed to talk to me like that, but regardless, the cat was out of the bag!
The radiologist released me, I guess, because I made the plane to Salt Lake City… with a headache.
In Salt Lake, we met with close friends and business partners. I told a small few, trying not to initiate panic, but asking for prayer and still hoping it would all blow over.
The following Monday, the 22nd, I saw the neurosurgeon, and she was less jovial than our first meeting months before.
“Your tumor has grown over 50%. This is a much more serious situation than I originally thought. It is compressing one of the two main veins to the brain. If it continues to grow at this pace, it is life threatening. It is unclear, but it looks like it is close to pushing your right brain to the left, which will cause seizures, so this is becoming an urgent situation. I wouldn’t touch it with a ten-foot pole. I am sending you to a specialist a few hours south of here. I assume surgery is your only option. We made you an appointment for next Monday. Bring your husband. You will want him with you.”
She handed me 2ft x 3ft films to hand-carry to the specialist neurosurgeon in the Detroit area. It felt like the entire office staff was looking at me with a, “poor girl,” glance as I walked out, but it was probably just in my head. (“Just in my head” began a whirlwind of puns, humor which Chris and I enjoyed to relieve the weight of the situation.)
I got to the car, dumfounded. Opening the humongous envelope that held the films
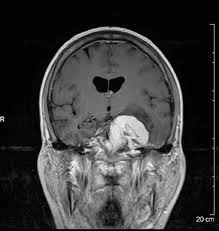
and spreading them across steering wheel, I could see a lot of gray matter – like any picture of a brain- except one big difference, the white, oblong golf ball on the side. It looked big for my small brain. I searched for my name and date to be sure they were really pictures of my brain.
As I drove home, my mind was silent. The chatter of “things to do today” was gone. The bother of the other drivers wasn’t registering on my new Richter scale.
.
Really? This could be IT?! The finish line is sooner than I thought?
But,… my “dash”?!
I remembered hearing Lou Holtz read the poem, “The Dash,” about the symbol on a tombstone between the birth date and the death date. The dash represented what was done with the life during the time on earth.
My dash may be done?! But I was going to make a difference in this world; I was going to raise my kids to be difference-makers; I was going to spread the Gospel: I was going to…
I drove past an abortion clinic, and I was reminded of how many in there didn’t have a chance to even start their dash. Life is not fair. I don’t deserve more than they.
What would I do differently? Ironically, that week I had just read the account of Hezekiah in 2Kings 20, where Hezekiah was granted another 15 years of life, after he was told he was dying. What would I do now if God chose to continue my dash?
In my quiet car that day, my priorities aligned, as if seeing a ghost of Christmas future and being pleased. What?! PLEASED? Yes, pleased. I did not think about where I could have been in the work place had I only held on to my position in engineering. I didn’t think of patents I could have owned or promotions I might have possessed. I realized more than ever that I was blessed to have invested the time of my dash (so far) into being a mom and wife and encouraging other moms and wives. I recognized the GIFT my husband gave me in being a stay-at-home mom! If God’s plan was that I would never speak again, I had no regrets of missed words with my children. I wish that for every woman who chooses to be a stay-at-home mom! If it were all over, I had no regrets.
I called Chris to let him know the doctor’s news, and by the time I arrived home 30 minutes later, he had a dozen coral roses on the kitchen counter, accompanied by his warm embrace.
As the week progressed to the appointment with the specialist neurosurgeon, my quiet times with the Lord progressed to depth. It is always during storms, when I seek the Son most.
Chris and I kept our secret, trying to protect our children, then ages 11, 8, 4 and 3 from fear. The night before the next neurosurgeon appointment, we decided to tell our parents of the impending days.
I had difficulty spitting the words out to my mother and father in Colorado, imagining they would feel helpless 1300 miles away, and fighting their own medical battles.
My mother immediately reacted as if packing her suitcase, “We will leave within the hour, and drive all night.”
I could barely keep her from hanging up the phone to pack, when I told them it was just a doctor’s appointment, and I would let them know if indeed surgery was scheduled.
Skull-base Neurosurgeon, September 29
“The fast growth rate of the tumor tells us it is likely NOT cancer; less than 4% chance.”
The appointment gained speed as the skull-base-meningioma specialist went through the options of treatment. “The brain surgery where the child is outside playing later in the day as seen in some commercial is not an option. The size of the tumor (3.6cm) exceeds the limits of our non-invasive radiation treatments. Waiting longer to see how the tumor acts [if it would shrink] is getting to a dangerous point, and we have zero data of a tumor that has ever grown at this rate and then stopped. In view of what lies ahead for you, if you have always wanted to go to Hawaii or something, now is a good time to go.”
I had never had to endure such a speech, and yet it continued.
“At your age and health, your body will handle the surgery well. However, due to the proximity to the vein, I don’t know that we will be able to get it all. I will use scissors so small that the tips can only be seen under magnification, but if even one cell is left, the tumor will grow back. Regular MRI’s will hopefully allow us to catch it small enough to use a radiation “knife” or other noninvasive options next time.”
He laid out a plan for future surgeries and radiation treatments dependent on my age at the time of diagnosis and size and growth rate of the tumor. This diagnosis did not look like it was ending… ever.
His informatory speech continued with how he would enter the cranial cavity (my head!) by cutting a football shaped piece, extract the tumor and then create a seal to replace the missing skull. The location of the tumor seemed to him far enough from the ear to be able to avoid hearing damage, but it looked like it was directly on the nerves of my mouth; one nick of a nerve would cause permanent paralysis and inability to use my mouth, so he would have a feeding tube team standing by for insertion.
“Is this why I have been choking?” I asked, grimly.
“The location could definitely cause swallowing problems.”
He continued to talk about the tumor’s location, also pressing on the main vein, as he gave us an anatomy lesson of the sinus vein and its relation to the body.
“I will not get close to touching that vein. I will get every cell I can –as long as it is not touching that vein. If it is nicked, bad things happen.”
My heart sank, knowing the tumor was visibly pushing on the vein in the MRI.
Chris excused himself, and I noticed that he, too, was going green in the face.
His absence didn’t stop the doctor’s progression.
“It is a two part surgery. The first is done by a vascular surgeon, who will go through an artery in your leg all the way to your brain, to put a “super glue” (for lack of a better word) into the tumor, to stave off bleeding. This pre-surgery often avoids the need of a blood transfusion. The second surgery is by my team, the following day. The head surgeon here [no pun intended] will want to be involved, due to the nature of your case, so we will schedule a day for both of us, although I am hoping only one will be needed.
You will be our only patient for the day. This second surgery will take 2-14 hours. You will be in ICU one night after the arterial procedure, then 1-2 more nights of ICU after the brain surgery, and 3-5 days in regular room. It usually takes two-three months to feel 80% healed and a year before patients feel 100%.”
It had been so long since I felt “100%,” a year didn’t seem like a long wait.
“So do you think this will take care of my headaches?” I asked, hoping he would give me a different answer than the last neurosurgeon.
“It’s hard to say, but the location of your headaches does not look related to where this tumor is. Unfortunately, I hate to say, but sometimes it can make headaches worse.”
I held the tears until Chris and I were alone in the car.
So let me get this straight:
– If I leave the tumor alone, its growth will likely lead to seizures, paralyze me and end in death;
– If I have surgery, there is a chance of paralysis or death.
– If I go through the two surgeries and a hospital week, and IF I survive and happen to get myself back without paralysis, the chances are high, that I will not feel any better than I have for a year, and I may even feel worse.
– And this is likely not the last time to have to go through all this.
Surgeries were scheduled for October 14 and 15.
As I called my friends, it felt like I was dropping a bomb on each one. I hated to make the call, and yet, I found through their tears, the love of Christ in our friendships was shining. When talking with my friend, Tracey Avereyn, I was the one who broke down. Through tears, I tried to master the language of cry-talking. I said, “I know that all things work together for good, but is it sinful that I dread this SO much?!”
Being a sister in Christ, she didn’t hesitate to sharpen as iron sharpens iron, “Terri, even Christ went to Gethsemane.” In other words, even Christ asked that the cup be taken from Him, but yet He conceded to God’s will being done.
The Son of God does not shine so bright as when our world is in its darkest state.
I knew Jesus had been through worse.
…..……...to be continued…….
Related Articles:
- Out of My Mind (with a Brain Tumor) Part I (terribradyblog.com)
- Out of My Mind (with a Brain Tumor) Part III (terribradyblog.com)
- Humor Tumor, Out of My Mind (with a Brain Tumor) Part IV (terribradyblog.com)